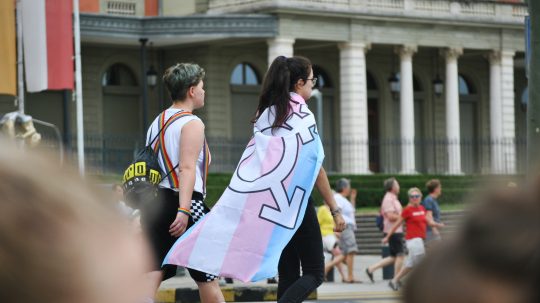On Trans Day of Visibility 2021, trans children in England and Wales may feel a little more visible, after a recent High Court decision confirmed that parents can consent to their children being prescribed puberty blockers and a court application will not normally have to be made.
On 26 March 2021, the High Court ruled in the parents’ favour – declaring that parents can consent to their children receiving puberty blockers, whether or not the child is Gillick competent. The Court also ruled that there was no general legal requirement to take these kinds of cases to court, meaning that where a parent consents to their child going on puberty blockers, court authorisation is not (usually) required.
Background
Trans is an umbrella term to describe people whose gender is not the same as – or does not sit comfortably with – the sex they were assigned at birth. Trans identities are diverse, and trans children and young people may identify in lots of different ways.
Some young trans people want to take puberty or hormone blockers to prevent puberty from happening because the changes it may bring to their body do not align with their gender identity. In some cases, this can ease their distress. In other cases, it can buy the person time to think about their gender identity. It may also prevent individuals from having to surgically reverse the physical effects of puberty if they later wish to transition genders.
The Gender Identity Development Service (GIDS), run by the Tavistock and Portman NHS Foundation Trust, is a clinic set up by NHS England to provide a gender identity development service for children and adolescents in addition to gender dysphoria services more generally.
GIDS takes referrals from England and Wales. Different services are available for children in Northern Ireland and Scotland. As the recent judgments involving GIDS were given by the High Court of England and Wales, they only apply to the legal position in England and Wales. Different (but similar) legal regimes operate in Northern Ireland and Scotland and the Scottish equivalent of GIDS said after the Bell decision that they would not be reviewing its services. Transgender NI’s statement can be seen here.

A transgender woman in a hospital gown speaking to her doctor (Credit: The Gender Spectrum Collection/Zackary Ducker)
Since 2011, GIDS has prescribed puberty blockers to under-16s who they consider are competent to consent to the treatment. This would only happen following multiple, months-long assessments, and with parental support.
In law, parents generally have the power and responsibility to consent to medical treatment on behalf of their children under 16-years-old. This is different for 16 and 17-year-olds who are presumed themselves to be able to give consent, which can only be overruled in exceptional circumstances.
Where a doctor is satisfied the child under 16 has sufficient maturity and intelligence to understand the nature of the treatment and its implications, the child is said to be “Gillick competent” and can consent to treatment in their own right. This follows a 1980s court case called Gillick v West Norfolk and Wisbech Area Health Authority.
The Bell v Tavistock decision
In 2019, two Claimants, Quincy Bell and Mrs A, challenged GIDS’ policy of prescribing puberty blockers (via two hospital Trusts) to individuals under eighteen. They argued that people under 18 years of age were not competent legally to give consent to taking puberty blockers. This case is known as Bell v Tavistock.
On 1 December 2020, the High Court gave its decision. The court said there were a number of things any child would have to be able to understand and weigh up before they could be considered legally competent to consent to puberty blockers. That included understanding the immediate physical and psychological consequences, the consequences of taking cross-sex hormones (because the court considered that would usually follow taking puberty blockers) and the “fact that the evidence base for this treatment is as yet highly uncertain”.
Importantly, the court said it was unlikely that under-16s would be able to give consent, given the different factors they would have to understand. In the court’s words:
“There will be enormous difficulties in a child under 16 understanding and weighing up this information and deciding whether to consent to the use of puberty blocking medication. It is highly unlikely that a child aged 13 or under would be competent to give consent to the administration of puberty blockers. It is doubtful that a child aged 14 or 15 could understand and weigh the long-term risks and consequences of the administration of puberty blockers.”
The ruling stymied GIDS’ practice of prescribing puberty blockers where it considered the under 16-year-old was competent because the court was saying that would rarely be the case.
What happened after Bell v Tavistock?
An hour after the Bell decision, the NHS changed its contract with GIDS so that:
- Patients under 16 could not be referred for puberty blockers unless a “best interests” order had been made by the Court
- Patients already taking puberty blockers must undergo a clinical assessment. If the clinician determines it is in the patient’s best interests to continue with puberty blockers, they must apply to the Court for a “best interests” order from the Court to confirm that is the case.
It appears that as of 1 December 2020, no new patients have been prescribed puberty blockers.
The AB Case
In January 2021, the parents of a 15-year-old transgender child, who started taking puberty blockers in July 2019, applied to court for a declaration that parents could consent to puberty blockers on behalf of their children, and no court order was required.
While more work still needs to be done, especially for trans children who do not have supportive parents to consent to treatment for them, the AB judgment is a welcome clarification of the law, highlighting that parents can consent to puberty blockers on behalf of their children, and a court application is the exception, not the norm.
On 26 March 2021, the High Court ruled in the parents’ favour – declaring that parents can consent to their children receiving puberty blockers, whether or not the child is Gillick competent. The Court also ruled that there was no general legal requirement to take these kinds of cases to court, meaning that where a parent consents to their child going on puberty blockers, court authorisation is not (usually) required.

(Credit: Sinitta Leunen)
What next?
The Good Law Project, which funded the AB case through its Trans Defence Fund, has written to the NHS requesting it to change its policy so that in cases where clinicians recommend puberty blockers to trans children and parents validly consent to the treatment, no court application needs to be made.
The letter highlights that this is urgent because trans children have been refused access to puberty blockers since 1 December 2020. It says “there is a cohort of children who are having to live with permanent developmental changes to their bodies that are inconsistent with their chosen gender”. (Some of the distress trans young people have gone through can be seen here and here.) At the date of writing, the NHS’s response is not known.
While more work still needs to be done, especially for trans children who do not have supportive parents to consent to treatment for them, the AB judgment is a welcome clarification of the law, highlighting that parents can consent to puberty blockers on behalf of their children, and a court application is the exception, not the norm. Meanwhile, the Bell judgment is being appealed, and the outcome may yet prove helpful for transgender children who do not benefit from their parents’ support.