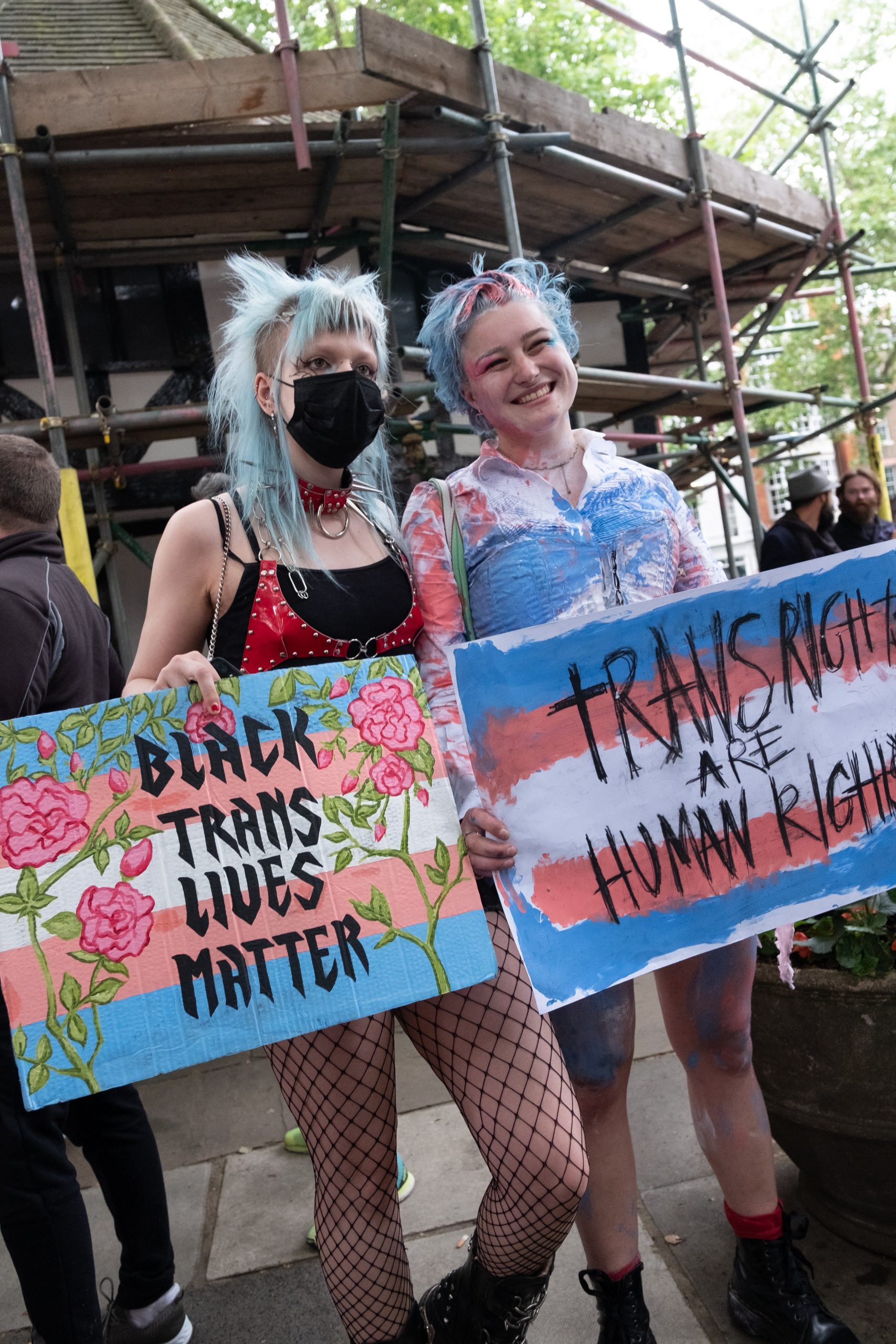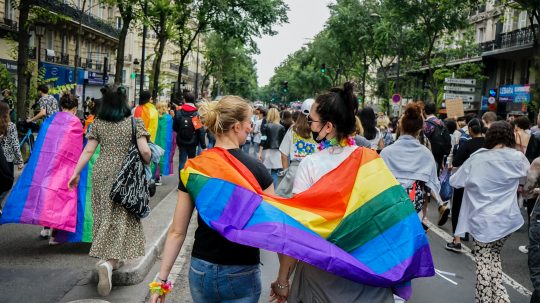Last month, the Equality and Human Rights Commission wrote to the Scottish government asking it to pause plans to reform the gender recognition process north of the border. We explore how this intervention and other recent developments relate to transgender people’s right to health in the UK.
The Equality and Human Rights Commission (EHRC), which is the UK’s equalities watchdog, wrote to the Scottish government saying that “more detailed consideration” was required before introducing a new, simplified system which would enable transgender people to change the sex recorded on their birth certificate.
The EHRC’s letter was widely critiqued by lesbian, gay, bisexual, trans and queer (LGBTQ+) equality campaigners as an unnecessary and worrying move. LGBTQ+ rights charity Stonewall said: “We are deeply troubled by the approach that the EHRC is taking to trans people’s human rights. Their approach appears to focus on pleasing a noisy minority of anti-trans activists, rather than promoting human rights for all LGBTQ+ people.”
Updating the Gender Recognition Act (GRA) to enable smoother transitions for transgender people has been the subject of debate for some time. Lack of progress in this regard, campaigners argue, poses a threat to transgender people’s right to health, as outlined by the UN and the International Covenant on Econmic, Social and Cultural Rights. The EHRC’s intervention has also been criticised as interfering with transgender people’s right to freedom from discrimination, protected under Article 14 of the Human Rights Act.