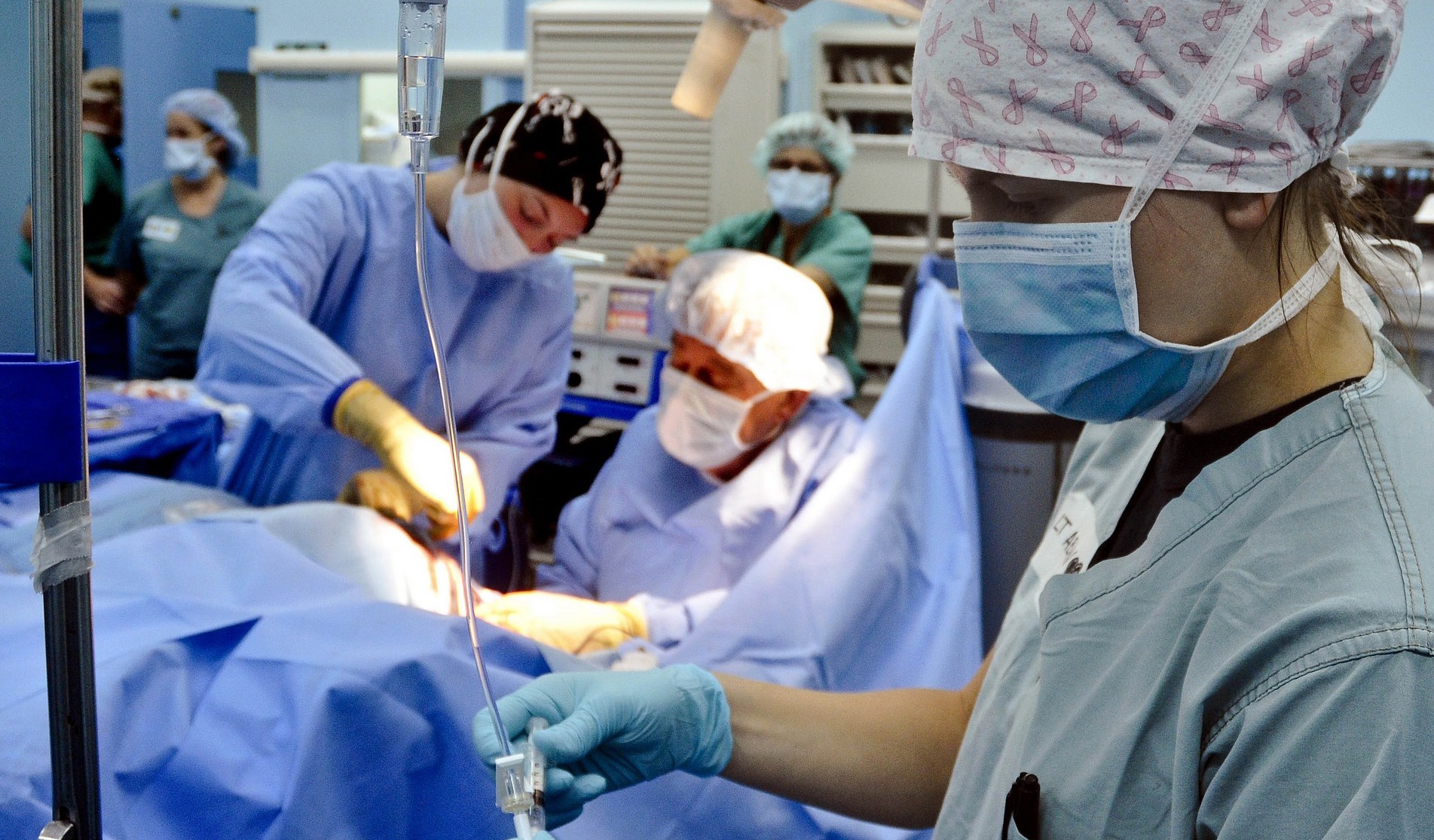
You’ve probably experienced it before. When you visit a doctor, they’ll check with you whether it’s OK for them to examine you, and then again when they suggest a course of treatment.
This is called consent to treatment, and it’s the principle that a person must give permission before they receive any kind of medical treatment, test, or examination. It applies to everything, from getting your blood pressure taken at the GP’s, right the way through to undergoing a major operation. It’s a crucial part of medical ethics and law, and of human rights law.
How does it work?
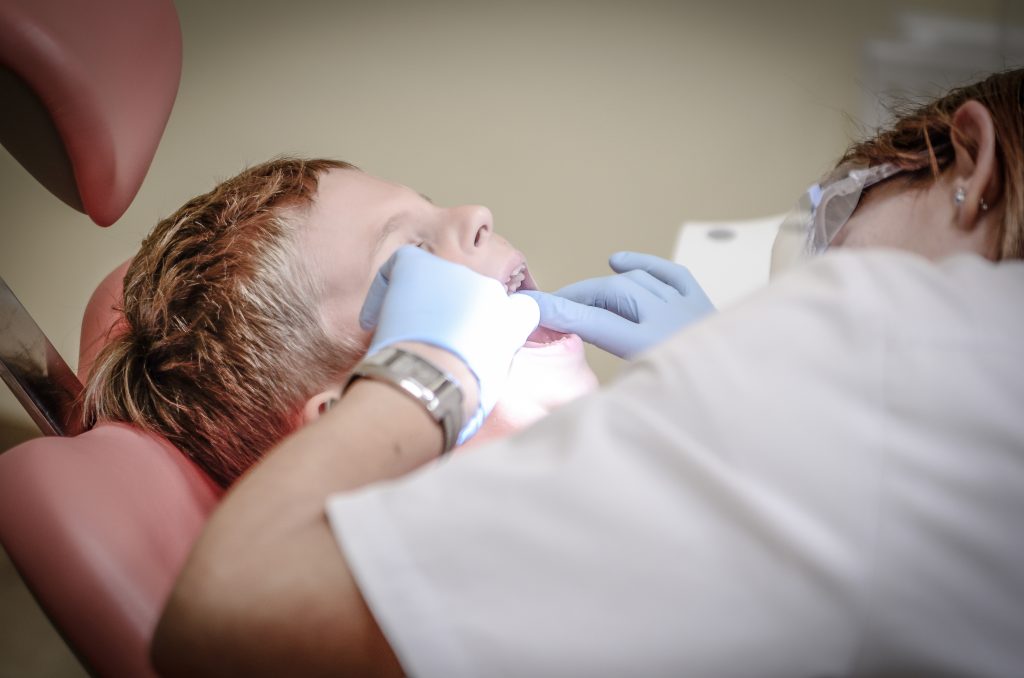 Image Credit: Pexels
Image Credit: Pexels
Consent is required any time a doctor wishes to examine and treat a patient. There are only a handful of exceptions to this rule, such as where someone requires emergency medical treatment to save their life, or where the law says it can be done to prevent the spread of an infectious disease.
For consent to be valid, it must comply with three requirements:
- It must be voluntary, meaning that the decision must be made by the individual themselves, without any influence or pressure from medical staff, family or friends;
- It must be informed, meaning that the individual must have been given all of the information they need in order to make their decision; and
- The person making the decision must have capacity, meaning that they must be capable of understanding and using the information provided to them to make a decision.
Why is it so important?
 Image Credit: Skeeze/Pixabay
Image Credit: Skeeze/Pixabay
Consent is an expression of respect for the right to self-determination and autonomy. It means that we think that individuals are the best people to make decisions about themselves, for themselves, and that they shouldn’t be subjected to treatment that they don’t want.
It’s so important that, if someone who has capacity refuses medical treatment, that has to be respected – even if it may result in serious injury or death. The courts have said that the right to self-determination exists regardless of whether a decision is one that others might view as irrational.
It’s not hard to find examples in history of the horrifying consequences of a lack of respect for consent, or of how human rights have helped: the brutal experiments carried out by the Nazis on concentration camp prisoners in the name of medicine and science was a key contributor in the development of human rights after the Second World War.
Why else are human rights important to medical consent?
 Image Credit: Clem Onojeghuo / Unsplash
Image Credit: Clem Onojeghuo / Unsplash
There are plenty of other ways human rights come into this too, with several parts of the Human Rights Convention coming into play. Here’s how.
Article 3 – Right to freedom from torture or inhuman or degrading treatment
The consequences of medical treatment without a patient’s consent could, in some circumstances, be considered to be inhuman or degrading. This was established by the Human Rights Court in a case called Herczegfalvy v Austria, where a man called Mr Herczegfalvy was given sedatives and other medical treatment without his consent in a psychiatric hospital. The court agreed that treatment without consent could, in theory, breach Article 3, but said that in this case Mr Herczegfalvy’s treatment hadn’t reached that stage. To show that medical treatment breached Article 3, it had to be shown that the harm met a minimum level of severity, and that the treatment wasn’t medically necessary.
Article 5 – Right to liberty and security
In the UK, the Mental Health Act can be used to admit someone to hospital and hold them for treatment against their wishes. It can only be used in respect of someone who is so seriously unwell that they must be detained in order to keep themselves or others safe. This is sometimes referred to as being “sectioned”.
Article 5 of the Human Rights Convention protects individuals against arbitrary detention, but there are exceptions. Article 5(e) permits the detention of “persons of unsound mind”, as long as the proper procedures are followed. Article 5 could therefore be used to challenge compulsory detention and treatment if the proper processes haven’t been followed.
One of the UK’s most senior judges, Mark Hinchcliffe, has recently questioned whether the law in relation to people with mental illness is correct. He suggested that, as long as someone’s mental disorder has not affected their capacity to make decisions, they should “have the right to self-determination, even if their decisions seem unwise.”
Does [the law] embody the sort of respect and regard for modern principles of non-discrimination, autonomy, personal choice and self-determination that, in this day and age, should underpin the way we look at someone with a mental health problem?
There’s an argument that the Article 14 right to freedom from discrimination is relevant to consent as well.
Article 8 – Right to respect for private and family life

Image Credit: London Scout / Unsplash
The Human Rights Court has confirmed that Article 8 protects our physical, moral and psychological integrity, as well as our right to choose. Failing to respect someone’s competent refusal of medical treatment, and providing treatment against their will, is therefore protected against by Article 8.
In Glass v United Kingdom, doctors treated a severely mentally and physically disabled boy against his mother’s wishes. (In the UK, parents can consent on behalf of children and young people). The Court found that the doctors’ decision to override the mother’s objection to the treatment had breached Article 8. Article 8 was also used to make arguments on behalf of the parents in the recent tragic case of Charlie Gard.
To be valid, consent must be informed. So if a patient consents to treatment on the basis of misleading information, or where information was withheld from them, it could be argued that treatment breached Article 8. This doesn’t mean that doctors must tell patients about every possible complication of the treatment, but they must be able to show that they have taken into account the patient’s Article 8 rights and be able to justify withholding information.
Article 9 – Right to freedom of religious expression
Article 9 sometimes come into play in issues of consent to treatment if someone refuses treatment on the grounds of their religion. Most Jehovah’s Witnesses, for example, believe that the Bible tells them they can’t accept blood transfusions. As with other patients, if an adult with capacity refuses to consent to a blood transfusion, this should be respected.
One of the few cases involving the refusal of a blood transfusion by a Jehovah’s Witness came to court before the Human Rights Act, and didn’t consider human rights arguments. The court held that the child’s refusal should not be respected, because it resulted from undue influence from her mother. It would be interesting to see how a court dealing with a similar case would weigh an individual’s Article 9 rights in making such a decision.
Want to find out more?
- Read more about how human rights laws have protected health in other cases.
- Look at our explainer on what it means to be “sectioned” under the Mental Health Act.
- Check out our beautiful infographics on each of the articles of the European Convention on Human Rights.