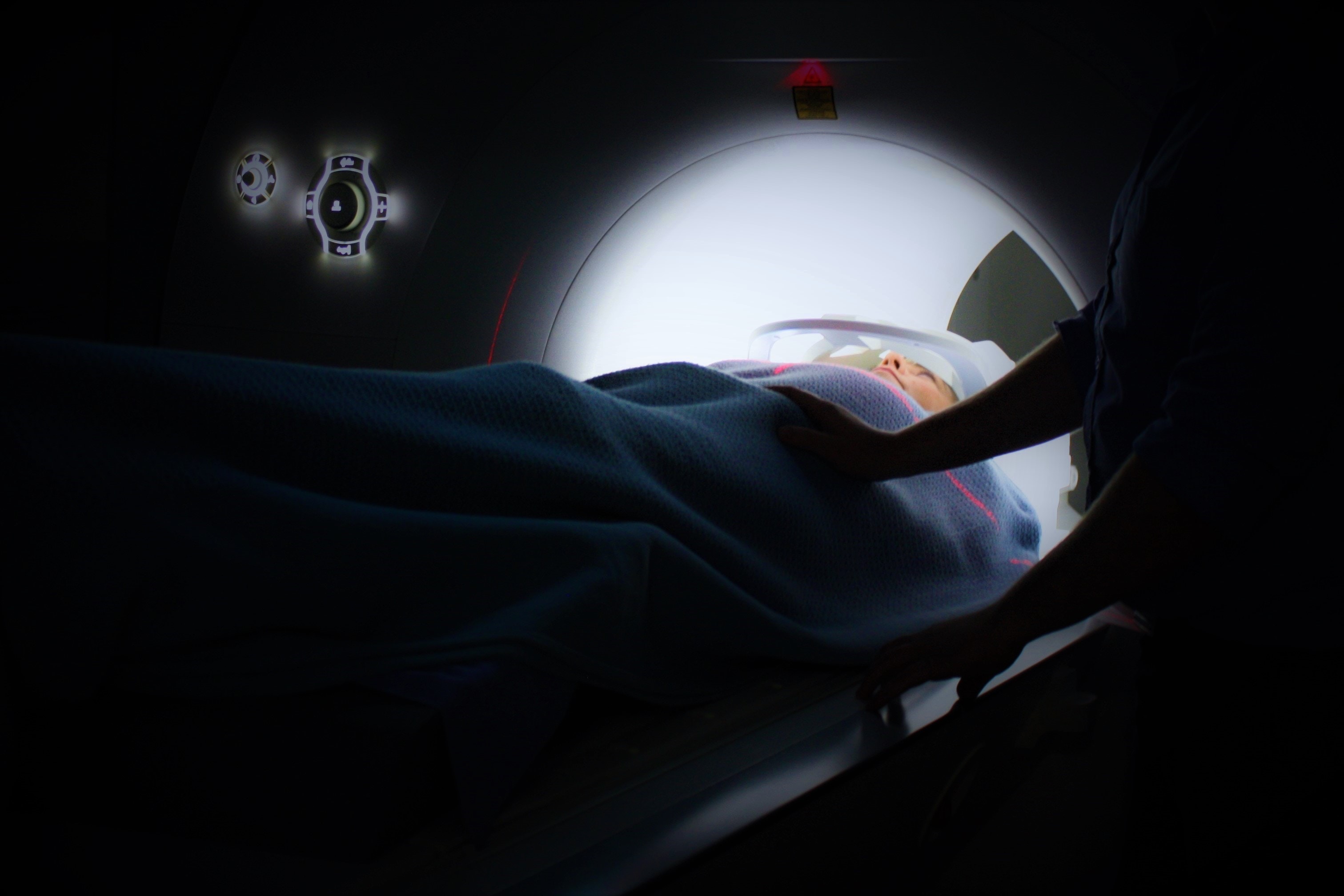
My Grandpa is getting old. Last year after a particularly bad fall, he spent four months in hospital.
The tall, slim man with coal black hair who used to be able to haul a whole sheep on his back across the family steading can’t move as quickly as he used to. His memory has been getting worse and worse – although he can still recall with alarming precision all of the grammar rules he learned at school.
When he was born in 1928, it would still be two whole decades before anyone had even heard of the NHS. His mother gave birth to him at home, with no doctor present so they didn’t have to pay for it.
A Growing Impact in Healthcare
 Image Credit: Public Domain Pictures / Pexels
Image Credit: Public Domain Pictures / Pexels
He’ll be 90 this year, and has lived through medical, technological, and social changes which have revolutionised healthcare.
He’s seen diseases eradicated, hip replacements, heart transplants, IVF, medical technology advancing at a rate unfathomable for someone born in a house without electricity.
What he might not realise – indeed he might be the first to tell you, despite my best efforts, that human rights are only for terrorists and criminals – is that he’s also been witness to the growing impact of human rights in healthcare throughout his lifetime.
Human Rights and Health
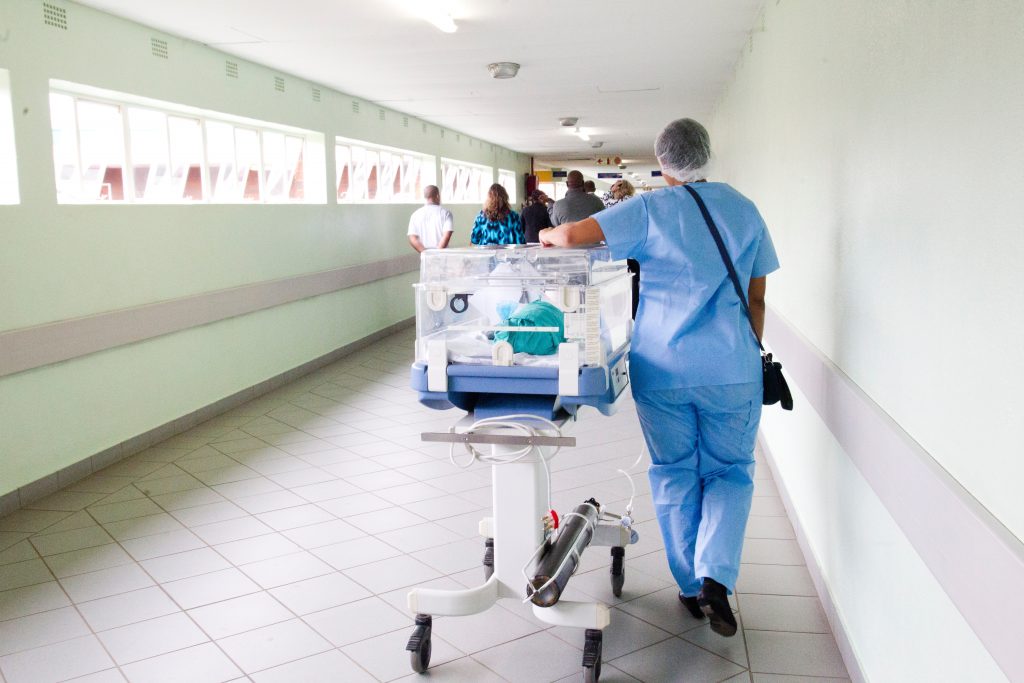 Image Credit: Hush Naidoo / Unsplash
Image Credit: Hush Naidoo / Unsplash
In celebrating his 90th birthday this year, my Grandpa will have outlived the life expectancy at birth for men born in the 1920s by over 40 years. Better access to healthcare and hospitals, the prevention and cure of treatable diseases, as well as better sanitation, diet and adequate housing have all played their part in recognising his right to the “highest attainable standard of health”.
He’s seen the birth of all three of his children and all five of his grandchildren in NHS hospitals, and his wife as the recipient of free maternity care, respecting fundamental rights to dignity, autonomy, privacy and equality.
The concept of mental health care would have been alien to him as he watched his father crippled with what we now know as post-traumatic stress disorder after carrying stretchers in the trenches of the First World War. It was only in the 1950s and 60s that Victorian psychiatric asylums were closed and mental health care as we know it now began to emerge. Today, not only do we have free mental health services on the NHS, we live in a society committed to breaking down the stigma surrounding mental health and ensuring dignity, respect and equality in mental health care.
He’s witnessed his daughter qualifying and practising as a doctor providing sexual and reproductive healthcare to everyone who needs it, supporting women to make choices about if, when, and how to have children.
Where he once had to accept the doctor’s knowledge and decisions unquestioningly, when he goes to see his local GP now he has the power and the autonomy to decide what’s best for him. Patients are now at the heart of care, empowered to make decisions for themselves and to speak up when things go wrong.
And last year, when things got bad, he was able to get the operations he needed when he needed them. He was cared for by all the hospital staff with the greatest dignity and respect. The very principles which now enable him to stay safely at home, surrounded by all the thing he loves: his piano; his Scottish country dance music radio show on at all full volume; his wife of over 60 years (though here’s where he’d get gruff and stoic and try to deny it in a way that only Highland men can).
Human rights under threat
![]() We have so much that we can and should celebrate. But there’s much more that must be done.
We have so much that we can and should celebrate. But there’s much more that must be done.
We’re living through an era of austerity. We hear reports daily about how the NHS is severely and chronically understaffed and underfunded. There’s a cost to this, one that comes at the expense of one of our most fundamental rights: a recent study estimated that spending cuts to health and social care were linked to 120,000 deaths in England.
We’ve just seen the worst winter crisis the NHS has ever experienced. My Grandpa had the operations and care he needed, but thousands of others had operations delayed or cancelled, or had to wait on trolleys in ambulances and hallways for hours before being seen, and hours more for a hospital bed. In the community, demand for general practice has reached levels which are “unmanageable and unsafe” for patients.
Mental health continues to be a “poor relation” in the NHS, with significant variability in funding, wait times, and treatments available across the UK. The consequences of this are severe: a recent report found “serious failings” in NHS mental health services, which, in extreme cases, had led to the deaths of patients. Failures in diagnosis and treatment, inappropriate hospital discharge and aftercare of patients, and a lack of dignity were all identified as “violating basic human rights”.
Respect, dignity, compassion. These are hallmarks of human rights but still sadly absent in so many cases: a woman in a psychiatric hospital forced to use a plastic cup instead of sanitary products during her period; patients left in soiled bandages or bedding for hours; abuse and neglect in nursing and care homes.
The NHS was created to provide healthcare that is “comprehensive, universal, and free at the point of delivery”. Yet this is not the reality for so many in socially excluded groups – those who are homeless, drug users, ex-offenders, those seeking asylum – who struggle to access healthcare and enjoy the benefits of good health. Inequality and poverty in the UK also have an impact on health: my Grandpa might be 90-years-old this year, but there are still parts of the UK where life expectancy for a man is just 54 years old. That’s not good enough.
Human rights save lives
My Grandpa has been lucky with his care. But it shouldn’t be about luck. What he has enjoyed in his 90 years should be available to us all.
We can’t get complacent. We can’t take what we have for granted. Everyone deserves what my Grandpa has had. And that’s why we need human rights in healthcare more than ever.